It was interesting to see the turnout for last night’s rural healthcare debate in the town hall – largely people who’d made the trip into Richmond from the more remote central and upper Dales areas of the district.
Interesting but, of course, not surprising, given they have particular issues facing them in the current re-organisation of the NHS – not least the challenge of retaining of GPs in practices which face losing central government funding and so may become unviable in the not too distant future.
But many other issues raised during the session hosted by William Hague MP showed up some concerns of wider interest, issues that are just as relevant whether you live in the town or up the dale.
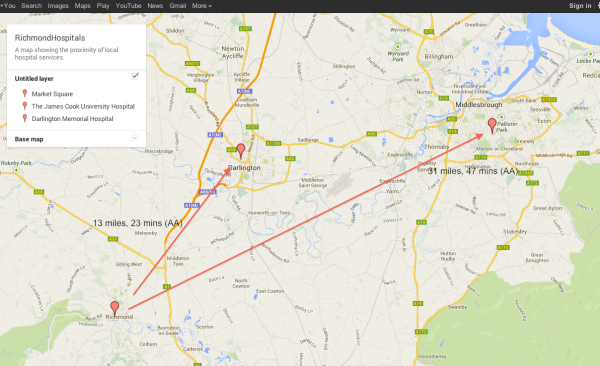
The first can probably be most easily illustrated with this diagram. Quite simply, where would you rather be rushed to in an ambulance or make the journey to for an outpatient appointment?
But the choice isn’t as simple as it first appears. The significantly closer Darlington hospital sits within a different administrative area and so patients’ records might not be made available in what’s seen as across a border (which most of us can’t see).
The experiences of two Swaledale residents who had been taken to Darlington hospital for treatment was relayed at the meeting and showed up this hidden danger of the necessary proceedures for sharing patient data not being in place.
The meeting heard the two had been admitted but their records couldn’t be shared so their relatives had to piece together their previous medical histories for doctors who were, to all intents and purposes, left treating them with no prior knowledge.
It was left to us all to imagine just how dangerous that could be in the case of people suffering life-threatening illnesses, on long-term medication and even those without relative advocates to assist them.
And talking of ambulances……
On the panel, Jo Harding, lead nurse and senior delivery manager, and Dr Mark Hodgson, GP and governing body member, both of the Hambleton, Richmondshire and Whitby Clinical Commissioning Group gave the presentation which you can listen to above.
One of the issues which it touches upon is the organisation’s poor record in ambulance arrival times.
The nationally set target says 75% should get there within eight mins but Ms Harding said that target hadn’t been achieved for a decade.
In a bid to address this problem, she said that an arrangement had been made with the Co-op store to have an ambulance responder based there in order to save time at the traffic lights.
This, she said, could potentially save one or two minutes of potentially life-saving time.
Various issues around that move weren’t raised at the meeting – what sort of equipment does the ‘responder’ carry? Why are ambulances waiting at lights at all? And crucially, what data has the decision been based on in terms of patient outcome if treated by a responder more quickly compared to waiting for a full ambulance a few minutes later?
The scheme only started last month so perhaps those are the questions for any future consultation. (Interested to hear your thoughts on this in the comments below as this also became quite a talking point on Twitter last night.)
But what about The Friarage…..
One of the biggest hospital issues locally is the proposed downgrading of services at The Friarage. Although William Hague touched on this in his opening remarks, which you can hear in the video above, debate on the topic was effectively taken off the table with the firm statements from the panel that the consultation period is over. We’ll have to wait until later this month to hear the next stage of that consultation.
There’s more reports from last night at:
– A campaign in Leyburn has been launched to fight plans to close an elderly care home and replace it with an extra care scheme.
– Summary of the meeting in The Northern Echo.
If we see any more, we’ll pop them on the noticeboard.